Seasonal Affective Disorder (SAD) is the scientific term for seasonal depression, most often occurring in winter. One can debate at length the relevance of the SAD concept, the pertinence and reliability of its diagnosis. Most importantly, some seasonal symptoms are observed among populations residing in the North of the Northern Hemisphere, where significant seasonal fluctuations in daylight duration prevail: low mood or decreased energy levels. SAD has been diagnosed since the mid-1980s. A seminal article from that era specifies: «During the winter affected individuals feel depressed, slow down, and generally oversleep, overeat, and crave carbohydrates.» (Rosenthal, 1985) Eventually, whether the occurrence of such symptoms is subsumed under the winter depression or SAD concept seems of little significance; for the sake of simplicity we will call SAD any combination of those symptoms: in short, winter mood and rhythm swings.
Winter sunlight
«Winter depression». What is «winter»? Seasons are primarily the effect of the tilt of Earth’s axis relative to the orbital plane of its rotation around the sun. This inclination causes, at a given latitude, a fluctuation during the year in day length and in sun angle – or equivalently, the altitude of the Sun at solar noon. In turn these affect the amount of heat energy received per Earth’s surface unit at a given latitude. Thus, «winter» is a seasonal «climate change» resulting from overall less heat energy per day per Earth’s surface unit from solar radiation, as a result of the low sun angle inducing more indirect, lower intensity light, as well as of reduced daylight hours.

Geographical cold
Climate of northern or polar regions therefore differs doubly from more southern or equatorial regions: i. the seasons there are more pronounced, which, as we have just seen, is the result of the Earth’s tilt on its axis; ii. these regions are also colder (generally, year-round). Here, the cause is not the Earth’s axial tilt, but the spherical shape of the Earth and its orbit around the sun (see Fig. 1)
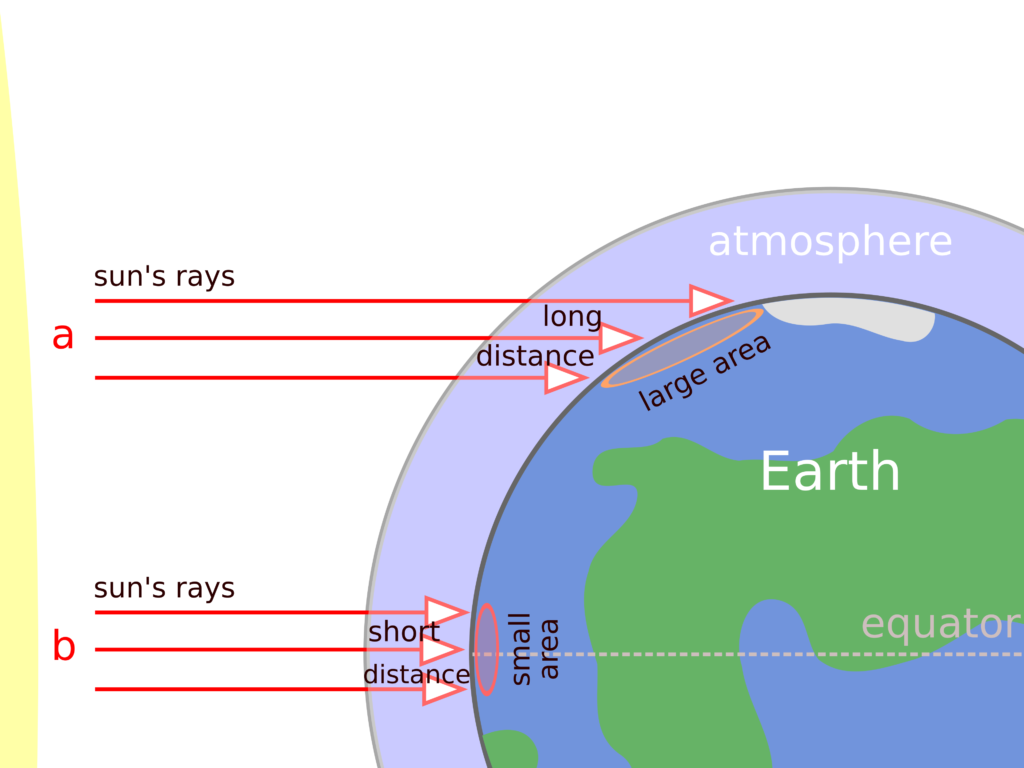
Winter depression must have as its cause or trigger «something that winter brings». It could be the cold and isolation. But the cold of the poles – relative to the south and the equator – is persistent and not seasonal. It seems to be established that winter sunlight – shorter daylight duration and dimmer light from a lower sun – is the major culprit.
From light to mood
The pioneering study by Rosenthal et al. mentioned previously intuited the importance of light in the development of seasonal depression. What put them on this track? Light is known as being an important «seasonal time cue in animals». As a result of their investigation, the authors «found that winter depression improved when patients were exposed to bright full-spectrum light before dawn and after dusk, thereby extending the photoperiod.» If tweaking the photoperiod – the duration of bright light exposure during the day – helps with winter depression, light must be closely linked to the phenomenon. (Rosenthal, 1985)
⋙ Read about light therapy for Seasonal Affective Disorder
Along which biological pathways would light and photoperiod influence mood?
Life on Earth, from bacteria to complex organisms, is pretty much synchronized to a cycle of approximately 24 hours – a circadian rhythm. In animals, such a rhythm is not limited to sleep-wake cycles, but also appears at the level of biological processes in cells and organs. Although biological cycles are endogenous – that is, maintained by the organism itself in the absence of environmental stimuli – «powerful external stimuli [can] influence and fine-tune» them: «in humans the most powerful of these external stimuli has been shown to be daylight.» (Brainard, 2015) Light influences mood because it affects the circadian biological cycles of cells, organs, and bodily functions.
It is the practical effectiveness of light therapy treatment for SAD symptoms that ultimately reveals the close link between limited winter sunlight, circadian cycle disruption, and winter depression. A study (Lewy, 2006) formulates and tests the so-called phase-shift hypothesis.
Circadian biology and sleep/wake cycles mismatch
«The PSH [Phase-Shift Hypothesis] postulates that most SAD patients become depressed in the winter because of the later dawn, causing their circadian rhythms to delay with respect to clock time and with respect to the sleep/wake cycle.» The correction of this phase delay through light therapy is significant and strongly correlated with improvement in seasonal depression. Nevertheless, this correlation is not sufficient, the study authors note, to prove the causal link between phase-shift and SAD – in other words, the important «circadian component of SAD». (Lewy, 2006)
What does it mean precisely for «circadian rhythms to delay with respect to clock time and with respect to the sleep/wake cycle»? How do we assess «circadian rhythms» and their «delay»?
Melatonin as an evidence
The most commonly used marker for assessing endogenous circadian phase position in humans is a marker of the time for the (circadian) evening rise of plasma melatonin levels. (Lewy, 2006; Terman, 2001) More precisely, this marker is the dim light melatonin onset (DLMO), as we sample plasma levels under conditions of dim light to avoid suppression of its production, with a plasma level threshold usually set at 10pg/ml. (Fig. 2)
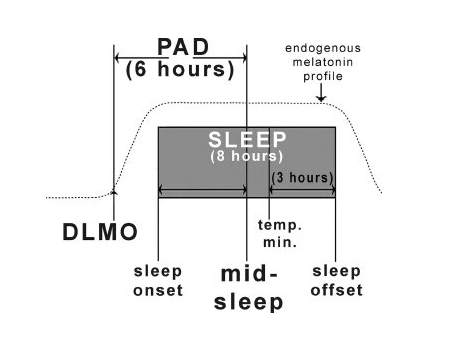
Ultimately, patients with winter depression most generally exhibit altered onset duration and offset of melatonin secretion as compared to healthy subjects – typically, a later DLMO and thereby a shorter phase-angle difference (PAD), defined as the interval between DLMO and mid-sleep. (Lewy, 2006; Terman, 2001)
Not only light therapy helps, Lewy shows, but also melatonin administration – the «chemical signal of darkness» – typically taken in the evening for the majority of patients who present a DLMO delay (while a minority presents a DLMO advance and would benefit from morning melatonin). This confirms that light therapy mitigates SAD via the mitigation of circadian rhythm disruption – in other words, it confirms the circadian component to SAD. (Lewy, 2006)
⋙ Read about light therapy for Seasonal Affective Disorder
Circadian pacemaker
We said that the melatonin production cycle «marks» circadian rhythm. But which circadian cycles are involved in winter depression and through what pathways are they impacted?
We must look first at a small region of the brain in the hypothalamus that is proven to be the circadian rhythms orchestrator or pacemaker: the suprachiasmatic nuclei (SCN). It is located just above the optic chiasm. Its neurons fire on daylight. More precisely, «daylight stimulates melanopsin receptors in retinal ganglion cells and these cells transform the physical signal into an electrical signal that stimulates the [SCN’s] neurons». (Brainard, 2015)
The electrical signal activates intracellular signaling pathways that induce the transcription of circadian genes including Period (Per), Cryptochrome (Cry), Clock, and Bmal1 in the SCN and subsequently in all peripheral organs through neural and hormonal signals. These genes are transcribed and translated into circadian proteins (PER, CRY, CLOCK, BMAL1) that impact SAD directly by dysregulating neurotransmitter rhythms or indirectly via melatonin dysregulation and circadian phase misalignment. (McClung, 2007; Dang, 2024)
Note that further research nuances the orchestrating prerogative of the SCN and indicates a system of «peripheral clocks» that receive time-of-day information from the SCN to then fulfill tissue-specific regulation. Thereby «desynchronization not only occurs between the external environment and the SCN rhythm generator but also affects phase alignments between the different peripheral clocks.» (Edery, 2000)
Interestingly, literature also binds circadian genes expression to anxiety and mood disorders : there might be a circadian component in depression in general – not just the winter one. (Dang, 2024; Walker, 2020; Francis, 2023)
What causes winter depression?
Limited daylight duration and intensity, it seems, causes SAD via the deregulation of circadian rhythms. Research shows circadian disruption, more precisely a mismatch or phase-shift between biological circadian rhythms and the sleep/wake cycle causes SAD. Daylight in turn is a key stimulus to circadian timing systems via the activation of the SCN’s neurons.
Anything disturbing circadian clocks is then a potential cause or aggravating factor to SAD. In some studies melatonin administration corrects both circadian rhythms and SAD, so that a disruption in the pathways of melatonin production, and any cause for it, can be a further culprit.
But scientific literature hints at other environmental cues to physiological circadian clocks to reset and coordinate. Notably, the intertwining of meal time with circadian clocks is well documented. Late eating time could promote circadian rhythms disruption. (Klevens, 2025) Skipping breakfast might dysregulate biological clocks: «the first meal of the day, consumed at the beginning of the activity phase […] is a powerful “zeitgeber”, or starter of peripheral clock genes expression». (Jakubowicz, 2023) Most interestingly, some important nutrients could be such time giving cues as well. Is fatty fish an obvious cure to SAD?
References
Rosenthal, N. E., Sack, D. A., Carpenter, C. J., Parry, B. L., Mendelson, W. B., & Wehr, T. A. (1985). Antidepressant effects of light in seasonal affective disorder. American Journal of Psychiatry, 142(2), 163–170. https://doi.org/10.1176/ajp.142.2.163
Brainard, J., Gobel, M., Scott, B., Koeppen, M., & Eckle, T. (2015). Health implications of disrupted circadian rhythms and the potential for daylight as therapy. Anesthesiology, 122(5), 1170–1175. https://doi.org/10.1097/ALN.0000000000000596
Lewy, A. J., Lefler, B. J., Emens, J. S., & Bauer, V. K. (2006). The circadian basis of winter depression. Proceedings of the National Academy of Sciences, 103(19), 7414–7419. https://doi.org/10.1073/pnas.0602425103
Terman, J. S., Terman, M., Lo, E. S., & Cooper, T. B. (2001). Circadian time of morning light administration and therapeutic response in winter depression. Archives of General Psychiatry, 58(1), 69–75. https://doi.org/10.1001/archpsyc.58.1.69
Klevens, A., Taylor, M., Roecklein, K., & Wescott, D. (2025). 0041 Greater depression severity is associated with later circadian eating time in those with seasonal depression. Sleep, 48(Supplement_1), A18. https://doi.org/10.1093/sleep/zsaf090.0041
McClung, C. A. (2007). Circadian genes, rhythms and the biology of mood disorders. Pharmacology & Therapeutics, 114(2), 222–232. https://doi.org/10.1016/j.pharmthera.2007.02.003
Dang, T., Uzoni, A., Kim, K., Clark, K., Layne, J., Lim, A. S., & Dueck, H. (2023). Risk for seasonal affective disorder (SAD) linked to circadian clock gene variants. Biology, 12(12), 1532. https://doi.org/10.3390/biology12121532
Walker, W. H., Walton, J. C., DeVries, A. C., & Nelson, R. J. (2020). Circadian rhythm disruption and mental health. Translational Psychiatry, 10(1), 28. https://doi.org/10.1038/s41398-020‑0694‑0
Edery, I. (2000). Circadian rhythms in a nutshell. Physiological Genomics, 3(2), 59–74. https://doi.org/10.1152/physiolgenomics.2000.3.2.59
Francis, T. C., & Porcu, A. (2023). Emotionally clocked out: cell-type specific regulation of mood and anxiety by the circadian clock system in the brain. Frontiers in Molecular Neuroscience, 16, 1188184. https://doi.org/10.3389/fnmol.2023.1188184
Jakubowicz, D., Rosenblum, J., & Wainstein, J. (2023). Influence of fasting until noon (extended postabsorptive state) on clock gene mRNA expression and regulation of body weight and glucose metabolism. International Journal of Molecular Sciences, 24(8), 7154. https://doi.org/10.3390/ijms24087154